From Hospitals to Communities: How AI Ultrasound Is Reshaping the Breast Cancer Early Screening System

— On World Cancer Day
Every year, February 4 marks World Cancer Day. On this day, a set of sobering numbers is repeated around the world:
About 20 million new cancer cases each year, and nearly 10 million deaths.
A large proportion of these deaths are not due to a lack of effective treatments, but to one simple fact: the disease was found too late.
Across almost all cancer types, early detection is the most certain—and the most cost-effective—way to save lives.
Breast cancer is a典型例子:
When detected early, the five-year survival rate exceeds 90%. Once it progresses to an advanced stage, survival drops sharply.
The question has never been whether early screening is important.
The real question is: why, in the real world, are so many women still not being screened in time?
1. A Long-Underestimated Group: Women with Dense Breasts
In Asian populations, more than 40–60% of women have dense breast tissue.
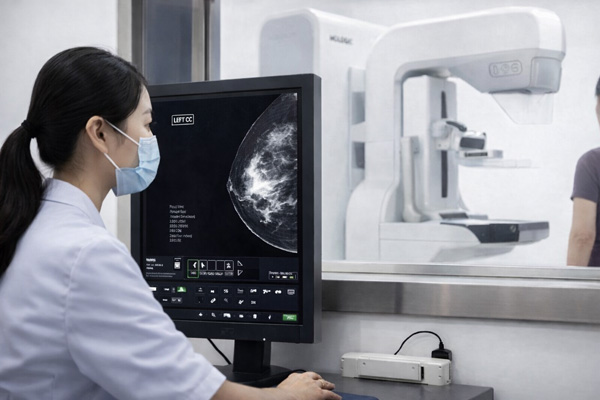
On X-ray mammography, dense tissue appears white—exactly the same color as most tumors. As a result, lesions can be “hidden” in the background.
This is not a problem of equipment quality, but a limitation of imaging physics and contrast.
Medical consensus is clear: the sensitivity of mammography drops significantly in women with dense breasts.
That is why in Japan, South Korea, and parts of Europe, ultrasound is officially recommended as an important complementary screening tool for this population.
2. Ultrasound Is the Right Tool—But Historically Not Scalable
From a technical standpoint, ultrasound is well suited for dense breasts:
- It directly visualizes soft tissue structures
- It is more sensitive to masses, nodules, and architectural distortion
- It involves no radiation and can be repeated frequently
- It is far less expensive than mammography or MRI
Yet ultrasound has always had a critical weakness: extreme dependence on the operator.
With the same machine and the same patient:
- Image quality varies from one examiner to another
- Interpretation of suspicious findings is highly subjective
- Miss rates correlate strongly with the examiner’s experience
This means that a tool seemingly ideal for primary care settings has, in reality, been difficult to deploy at scale.
You cannot realistically expect every community clinic, township hospital, or screening center to be staffed with highly experienced breast sonographers.
3. The Real Value of AI: Not Smarter, but Scalable
For years, discussions about AI in medical imaging have focused on one question: can it outperform experts?
In practice, a more important question is:
Can it turn expert-level capability into something that can be reliably replicated at scale?
In ultrasound, AI’s value is not mainly about detecting one or two more subtle lesions. It lies in three often overlooked dimensions:
1. Standardizing the scanning process
AI can guide operators in real time—confirming full breast coverage, identifying missing quadrants, and prompting additional sweeps of suspicious areas.
This addresses the question: Was the exam complete?
2. Providing consistent lesion alerts
AI can automatically highlight suspicious structures and assign risk categories.
This addresses the question: Did you notice what matters?
3. Lowering the experience barrier
When a nurse or technician with basic training can perform a qualified screening exam with AI assistance, ultrasound finally becomes deployable at the community scale.
4. From Hospitals to Communities: The True Breakpoint in Screening
A candid look at today’s screening system reveals a structural gap:
- Expertise is concentrated in tertiary hospitals
- High-risk populations are concentrated in primary care settings
- Equipment has moved downward
- Capability has not
The result is paradoxical: those who need screening the most often have the least access to high-quality screening.
AI combined with ultrasound does not merely change individual diagnoses—it reshapes the topology of the entire screening network.
It makes a practical model possible:
Low-cost ultrasound devices plus AI systems deployed in community clinics, primary hospitals, health check centers, and public screening programs;
standardized image acquisition by non-experts;
consistent AI-assisted interpretation;
and precise referral of high-risk cases to higher-level hospitals.
5. Not Replacing Doctors, but Fixing a Structural Shortage
Whenever AI in healthcare is discussed, a common misconception arises: Is it trying to replace physicians?
The reality is the opposite.
In breast cancer screening, the core problem is not physician replacement—it is physician scarcity. Skilled ultrasound specialists are in short supply worldwide.
AI’s role is closer to this:
- Turning scarce expert knowledge into a widely available baseline capability
- Converting variable, experience-dependent workflows into standardized ones
- Replacing the question “Do we have a top sonographer?” with “Do we have an AI-enabled system?”
6. On World Cancer Day: A Practical, Deployable Path Forward
Talking about AI on World Cancer Day should not be about showcasing technology. The real question is simple:
Can it help more people who would otherwise be missed get detected earlier?
For women with dense breasts, a realistic and actionable pathway is already clear:
- Use ultrasound as a primary screening tool rather than relying solely on mammography
- Use AI to remove dependence on highly specialized operators
- Extend screening from hospitals into community settings
- Shift from an “expert-scarcity model” to an “infrastructure model”
This is not a futuristic vision. It is an engineering and public-health project that can begin today.
World Cancer Day is more than a date of remembrance. It is a mirror, reminding us that what often determines life or death is not the most advanced therapy, but whether a patient is seen in time.
If AI-powered ultrasound can help more women be detected at an early, asymptomatic stage of breast cancer, its true value will not be measured by algorithmic metrics, but by the countless lives that can still be saved.


